HVAC system design for healthcare facilities is fundamentally an engineering discipline that directly impacts life safety. Unlike typical commercial spaces where only occupant comfort needs to be considered, healthcare HVAC must simultaneously satisfy multiple objectives including infection control, indoor air quality, specialized pressure differential requirements, and equipment heat dissipation. This article examines the core issues of healthcare HVAC design based on ASHRAE Standard 170 and relevant Taiwanese regulations.
1. Regulatory Framework for Healthcare HVAC Design
The internationally authoritative reference for healthcare HVAC design is ASHRAE Standard 170 -- Ventilation of Health Care Facilities[1]. This standard specifies in detail the minimum air change rates, pressure relationships, temperature and humidity ranges, and filtration efficiency requirements for various types of healthcare spaces. In Taiwan, the Ministry of Health and Welfare's Standards for Medical Institution Establishment and the Ministry of Interior's Building Technical Regulations (Building Equipment Chapter) also contain relevant provisions[2].
Notably, the 2021 revision of ASHRAE 170 further strengthened protection requirements against airborne infection, closely related to the lessons learned from the COVID-19 pandemic[3]. The updated standard places greater emphasis on outdoor air intake quantities, filtration efficiency, and exhaust air treatment, presenting new challenges for HVAC system upgrades in existing healthcare facilities.
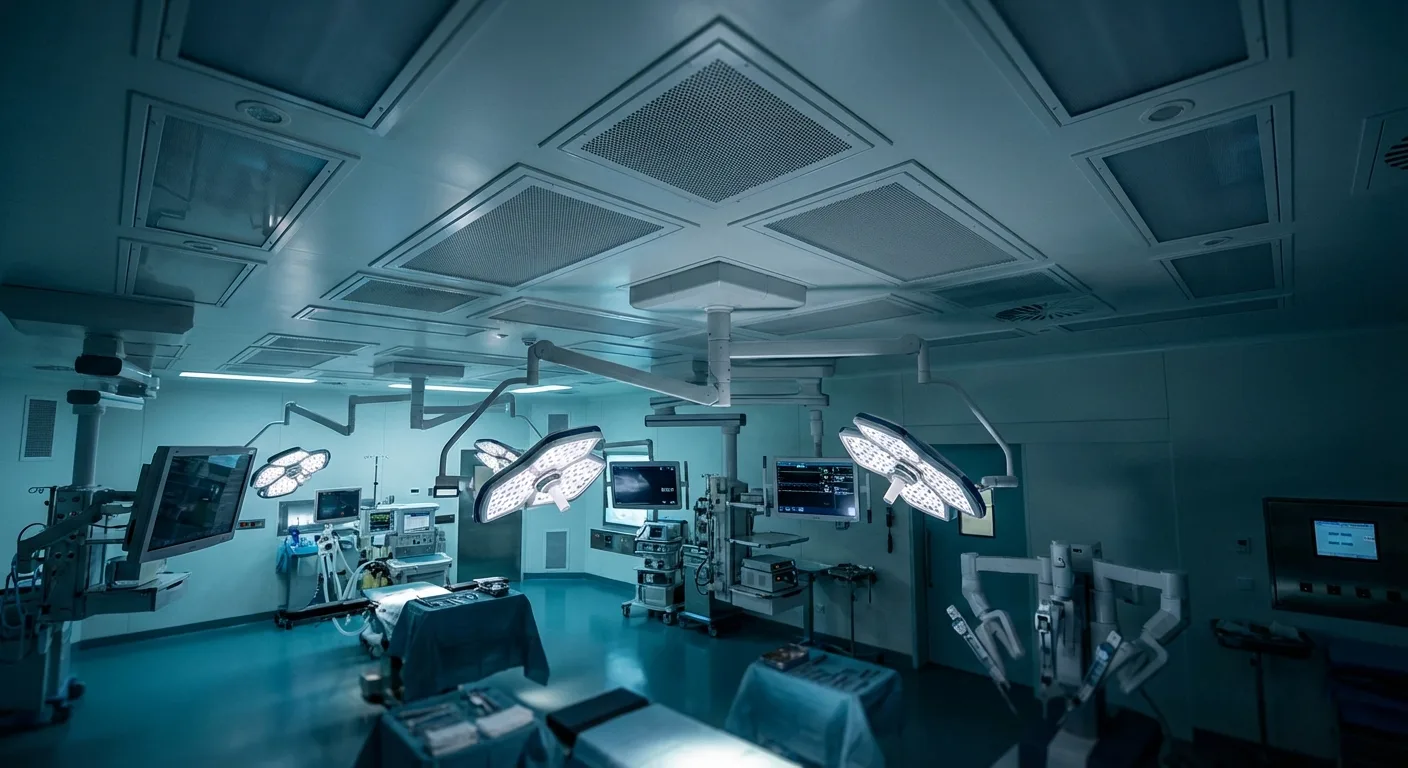
2. Operating Room HVAC: The Most Stringent Environmental Requirements
The operating room is the most stringently controlled space in healthcare HVAC design. ASHRAE 170 requires operating rooms to maintain positive pressure (at least +2.5 Pa relative to corridors), with a total air change rate no less than 20 air changes per hour (ACH), of which outdoor air changes must be no less than 4 ACH[4].
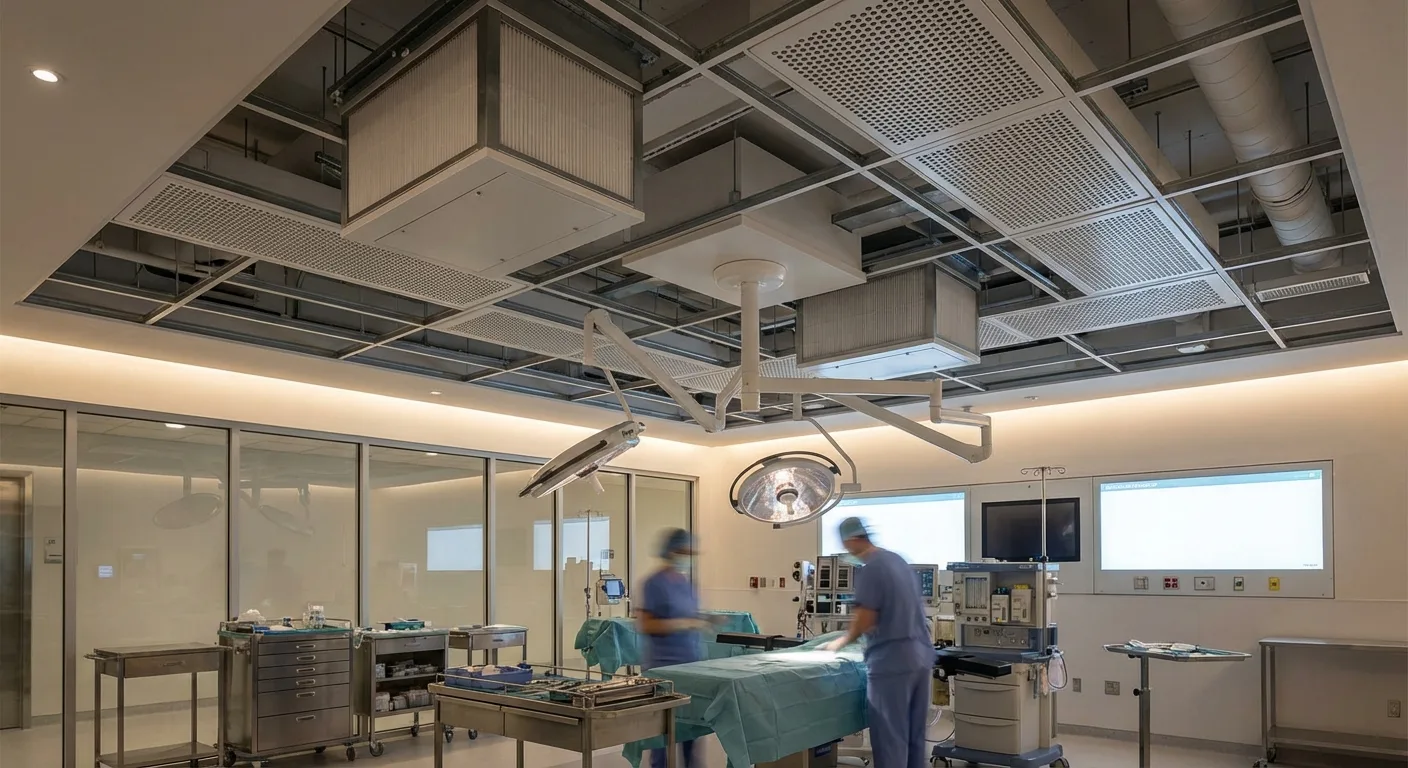
Laminar Flow Operating Rooms
For high-risk surgeries such as joint replacement and organ transplantation, laminar flow operating room designs are typically required. A large-area (approximately 2.4m x 3.0m) HEPA-filtered supply air panel is installed above the surgical zone, delivering unidirectional airflow downward to cover the operating table and surrounding critical areas[5].
Airflow velocity in laminar flow operating rooms is generally maintained at 0.2-0.3 m/s, with the supply air panel covering the central area of the surgical zone. During design, consideration must be given to the interference of surgical lights, surgical personnel, and various tubing on the airflow field -- these obstructions create wake effects, forming turbulent zones downstream that reduce local particulate removal efficiency[6]. Therefore, the selection and installation position of surgical lights must be closely coordinated with HVAC design.
Temperature and Humidity Requirements
Operating room temperatures typically range from 20-24 degrees C (adjustable based on surgical requirements), with relative humidity controlled between 30-60% RH[7]. Lower temperatures help reduce surgical team fatigue and lower wound infection risk, but must also account for the risk of hypothermia in anesthetized patients. Excessively low humidity increases the risk of electrostatic discharge (ESD), affecting the normal operation of electronic instruments; excessively high humidity is unfavorable for keeping the surgical site dry.
3. Isolation Wards: The Choice Between Negative and Positive Pressure
The HVAC design of isolation wards depends on the purpose of isolation:
Airborne Infection Isolation (AII) Rooms
Used for patients with airborne infectious diseases such as tuberculosis, measles, and varicella. ASHRAE 170 requires AII rooms to maintain negative pressure (at least -2.5 Pa relative to corridors), with a total air change rate no less than 12 ACH (6 ACH for existing facilities) and outdoor air changes no less than 2 ACH[8]. Exhaust air must be discharged directly outdoors or HEPA-filtered before recirculation.
During the COVID-19 pandemic, many healthcare institutions faced insufficient numbers of negative pressure isolation rooms. The US CDC and ASHRAE provided interim conversion guidelines for this scenario, including the use of portable HEPA air purifiers to increase the equivalent air change rate of existing rooms[9].
Protective Environment (PE) Rooms
Used for immunocompromised patients, such as those who have undergone bone marrow transplantation. PE rooms require positive pressure (at least +2.5 Pa relative to corridors), with a total air change rate no less than 12 ACH, and supply air must be HEPA-filtered (H13 or above)[10]. Some healthcare institutions even require PE rooms to achieve ISO Class 7 cleanliness standards.
4. Multi-Stage Filtration System Configuration
Healthcare HVAC systems typically employ a multi-stage filtration architecture. ASHRAE 170 specifies that supply air for general healthcare areas must pass through at least two stages of filtration[11]:
- First Stage: MERV 7 (minimum), installed at the air handling unit intake section, capturing large particles and protecting downstream equipment
- Second Stage: MERV 14 (minimum), installed downstream of the supply section, capturing fine particles
- Third Stage (Special Spaces): HEPA (99.97% @ 0.3 um), used for operating rooms, PE rooms, and other high-requirement spaces
The MERV (Minimum Efficiency Reporting Value) classification is based on ASHRAE Standard 52.2[12]. MERV 14 achieves 75-84% filtration efficiency for 0.3-1.0 um particles and exceeds 90% for 1.0-3.0 um particles. For spaces requiring higher protection levels, MERV 16 (efficiency of 95% or greater for 0.3-1.0 um) can serve as an alternative to HEPA.
5. Outdoor Air Treatment and Energy Balance
A key characteristic of healthcare HVAC systems is their high outdoor air ratio. To maintain indoor air quality and positive pressure requirements, outdoor air volumes for many healthcare spaces range from 20% to 100% of total supply air volume[13]. In Taiwan's subtropical climate, the cooling and dehumidification energy required for outdoor air treatment accounts for a significant proportion of total HVAC system energy consumption.
To balance indoor air quality and energy-saving objectives, the following strategies are worth considering:
- Application of Energy Recovery Ventilators (ERV) to recover sensible and latent heat from exhaust air
- Introduction of Dedicated Outdoor Air Systems (DOAS) to separate outdoor air treatment from indoor load conditioning
- CO2 concentration sensor-linked Demand-Controlled Ventilation (DCV), adjusting outdoor air volume based on actual occupancy density in non-surgical or non-isolation areas
However, caution is needed when applying energy recovery ventilators in infection control areas -- any risk of cross-contamination between exhaust and intake air would violate the fundamental principles of infection control[14].
6. Backup Systems and Resilient Design
Continuous operation of healthcare HVAC systems is critical to patient safety. For critical spaces such as operating rooms, intensive care units (ICUs), and negative pressure isolation rooms, the HVAC systems must have backup capabilities. This includes:
- N+1 redundancy configuration for chillers
- Dual-fan design or backup units for critical area air handling units
- Emergency power system capacity planning that covers HVAC loads for critical areas
- Fail-safe logic design for automatic control systems
Conclusion
Healthcare HVAC design is a complex discipline that must simultaneously address engineering science, infection control medicine, and regulatory compliance. Behind every air change and every pressure differential value lies a commitment to patient safety. As awareness of infectious disease risks increases and medical technology advances, the design standards in this field will continue to evolve. As HVAC engineers, we have a responsibility to work closely with healthcare teams, applying the most rigorous engineering principles to safeguard every healthcare space.